[ad_1]
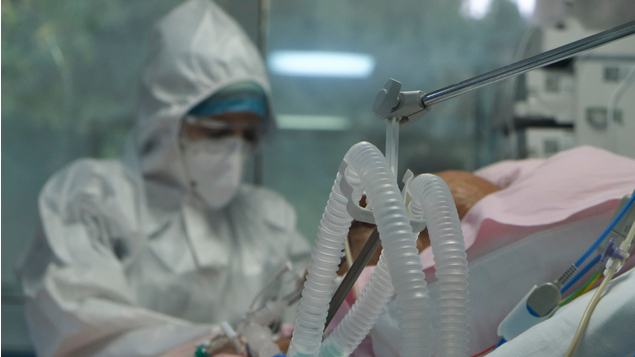
Shutterstock
More than one in three (35%) Covid-19 patients who are put on a ventilator experience symptoms of post-traumatic stress disorder (PTSD).
A study, conducted by Imperial College London and the University of Southampton, also found PTSD symptoms prevalent in 18% of people who were hospitalised with Covid-19 but did not require a ventilator; and 16% of people who were given medical help at home.
Those who required no help at home but experienced breathing problems linked to Covid-19 infection also reported PTSD symptoms, but to a lesser extent (11%).
The study’s authors suggest that adequate mental health support will be of “paramount importance” to their recovery.
Some 13,000 people were surveyed for the study, which has been published in the BJPsych Open journal. They answered an adapted a clinical questionnaire which had 10 questions on symptoms of PTSD most relevant to Covid-19, including intrusive images, trying to “erase” memories, and being easily startled.
Thirty-five per cent put on a ventilator experienced all 10 of these symptoms and 41% of all participants experienced at least one symptom to an “extremely” high degree.
“Intrusive images”, or flashbacks, was the most common symptom of PTSD in those requiring hospital ventilator support.
Dr Adam Hampshire, from Imperial College London’s Department of Brain Sciences, said: “We can see that the pandemic is likely to be having an acute and lasting impact, including for a significant proportion of patients who remained at home with respiratory problems and received no medical help. This evidence could be important for informing future therapy and reducing the long-term health burden of this disease.”
Professor Sam Chamberlain from the University of Southampton’s Faculty of Medicine said: “This study adds to mounting evidence linking Covid-19 to population-level negative mental health effects and shows that these can be measured conveniently in the general population using innovative digital methodologies.”
[ad_2]
Source link