[ad_1]
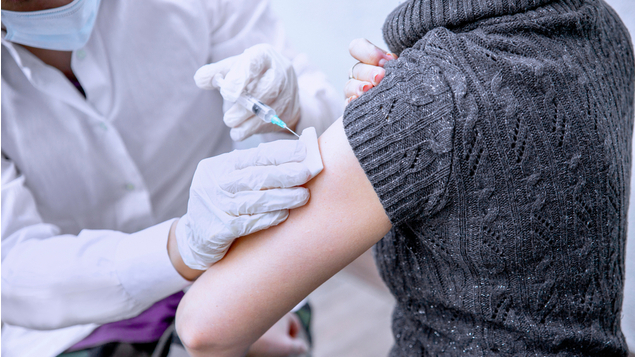
Shutterstock
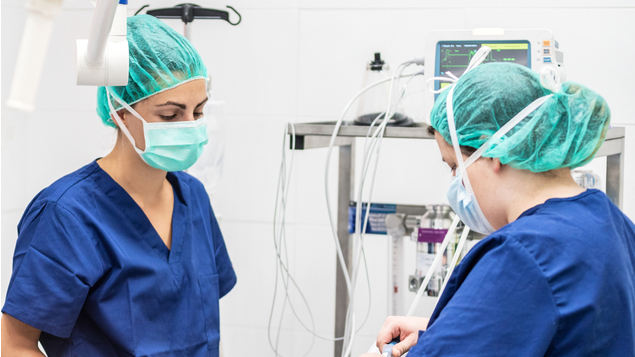
With the UK’s Covid-19 vaccine rollout now underway, the arrival of a potentially life-saving jab is no longer a dream. While things have gone well so far, the scale of the logistical challenge – including correct storage protocols – should not be underestimated, as Mike Butt explains.
All of us, from locked-down families to businesses to hard-pressed NHS staff, are placing huge store in the nation’s Covid-19 vaccine rollout. Every single jab administered brings with it the promise of life returning to some kind of normality.
However, despite the early – and, it has to be said, impressive – success of the rollout programme so far by the NHS and government, it also needs to be noted that the purchase costs of this eagerly awaited programme have placed a considerable additional burden on the NHS’s overall vaccine budget (currently around £200m a year).
About the author
Mike Butt is managing director at LEC Medical
Therefore, any contribution to mitigating the pressures on already overstretched health and social care budgets is to be welcomed. And one important mitigation is avoiding waste caused by mistakes in transport, logistics or storage.
Much has been written about the “last mile” of the cold chain challenge, specifically in its relation to the Pfizer/BioNTech vaccine, because of its very low temperature requirements. But perhaps not enough consideration has been given to the challenge of keeping the vaccine cool at the point of administration.
So, why does this matter?
The impact of badly stored vaccines
The active chemicals in all vaccines and other medication can change in molecular form when exposed to different temperatures, and the front-running Covid vaccines from Pfizer, Moderna and Oxford/AstraZeneca are no different, despite the latter being much easier to store and refrigerate.
For example, measles and the combined MMR vaccines can have their potency reduced by higher temperatures, while the Hepatitis B and HPV vaccines are sensitive to temperatures which are too cold.
Vaccines naturally biodegrade over time and being stored outside their recommended temperature range may speed up this loss of potency.
This impact cannot be reversed, and a vaccine may then fail to create the desired immune response and give protection – an unthinkable scenario in the case of the Covid vaccination, of course.
Avoiding waste and protecting the public
The “cold chain” – or the cold transportation of goods – is designed to protect vaccines and other biologics from point of manufacture through their transportation to pharmacies, where they must be safely stored before being distributed to clinical locations such as GP surgeries.
As we have all heard since its approval in December, during this process the Pfizer/BioNTech vaccine must be kept extremely cold, at -70°C. The Moderna vaccine, too, needs to be frozen, in its case at -20°C.
However, even if the vaccines are safely transported, all of this is pointless if things go wrong in the final link of the chain – at pharmacies, hospitals and GP surgeries. Once delivered, all of the currently available vaccines can be stored for up to five days within strict 2-degree to 8-degree parameters.
Failure to store vaccines according to manufacturers’ strict temperature requirements can invalidate the expiry date and cause manufacturers to disclaim responsibility for any apparent failure of the medicine, as the safety and effectiveness of such medicines can be significantly compromised or unknown.
To minimise this risk, pharmacies and GP practices should therefore have named individuals responsible and accountable for the receipt and storage of vaccines and other heat-sensitive medicines, and the monitoring and recording of fridge and ambient room temperatures.
Crucially, refrigerators used for the storage of medicines must be designed specifically for that purpose.
Standard domestic refrigerators cannot be used for storing cold chain products for several reasons. These include an uneven temperature distribution (as a result of minimal air circulation) and a normal operating range of between 0°C and 10°C.
The refrigerator used must also be of an appropriate size for the quantity of stock to be stored, in other words filled to no more than 75% capacity to allow adequate air circulation. It must also be reserved exclusively for the storage of vaccines and other pharmaceutical products, and so not used to store food, blood, milk, drink, or anything else representing a contamination risk.
Care must also be taken to ensure the refrigeration unit is sited in a well-ventilated room maintained between 10°C and 25°C, away from external windows and all heat sources, for example radiators or direct sunlight, and at least 5-10 cm from walls and other units.
To ensure its ongoing effectiveness, any vaccine refrigeration unit must be serviced according to manufacturer’s instructions and have its integral thermometer independently calibrated to ensure readings are true.
Finally, the medical refrigerator must be cleaned regularly, and the internal stock should be stored according to first expiry.
Maintaining public trust
The World Health Organization (WHO) has called “vaccine hesitancy” one of the top 10 threats to global health.
There are huge challenges here around tackling online misinformation. Just as critical in maintaining public trust and confidence, however, is ensuring it is very clear that Covid-19 vaccines are being transported, stored and delivered safely, so as to ensure their efficacy and avoid waste.
Medical settings (including, hopefully in time, occupational health settings as we move through the vaccination programme later this year) can play a small but significant part in maintaining that fragile public trust.
The Covid-19 pandemic has shone fresh light on the vital role that vaccines play in maintaining healthy communities, taking pressure off overburdened health services, and keeping economies afloat.
The scale of this vaccine rollout, both in the UK and across the world, is unprecedented. As hospitals find themselves under increasing pressure, arguably it has never been more important for us all to be ensuring we are communicating, emphasising and embedding good practice in our daily practices and procedures to ensure not one batch of vaccines is wasted.
[ad_2]
Source link